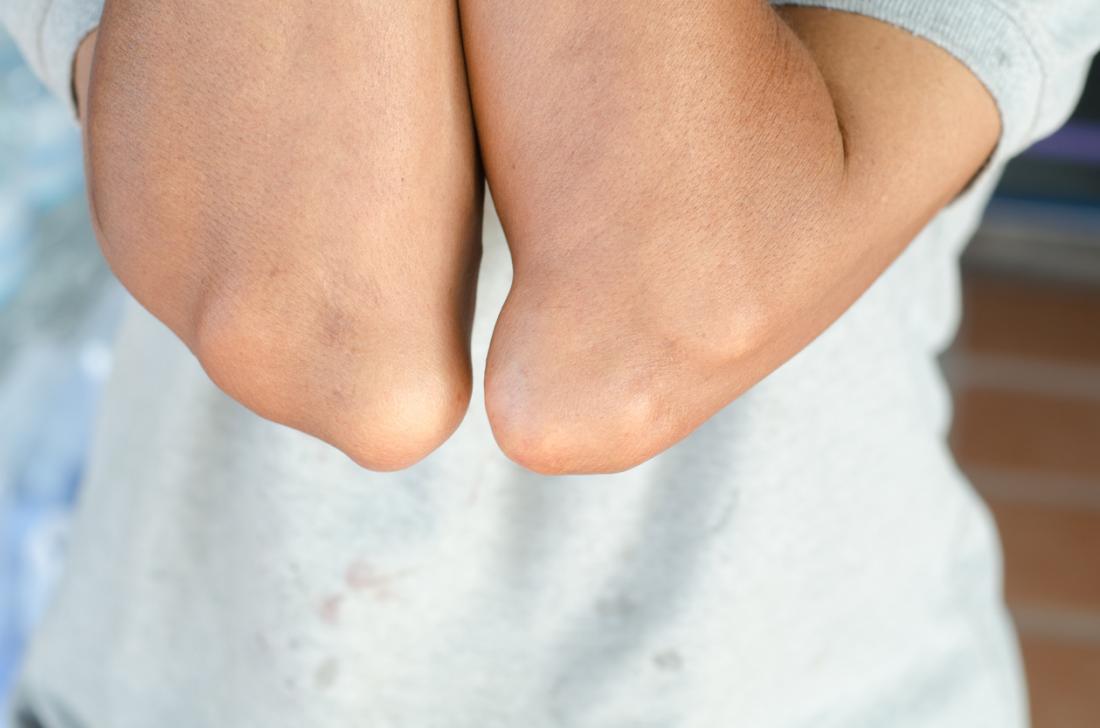
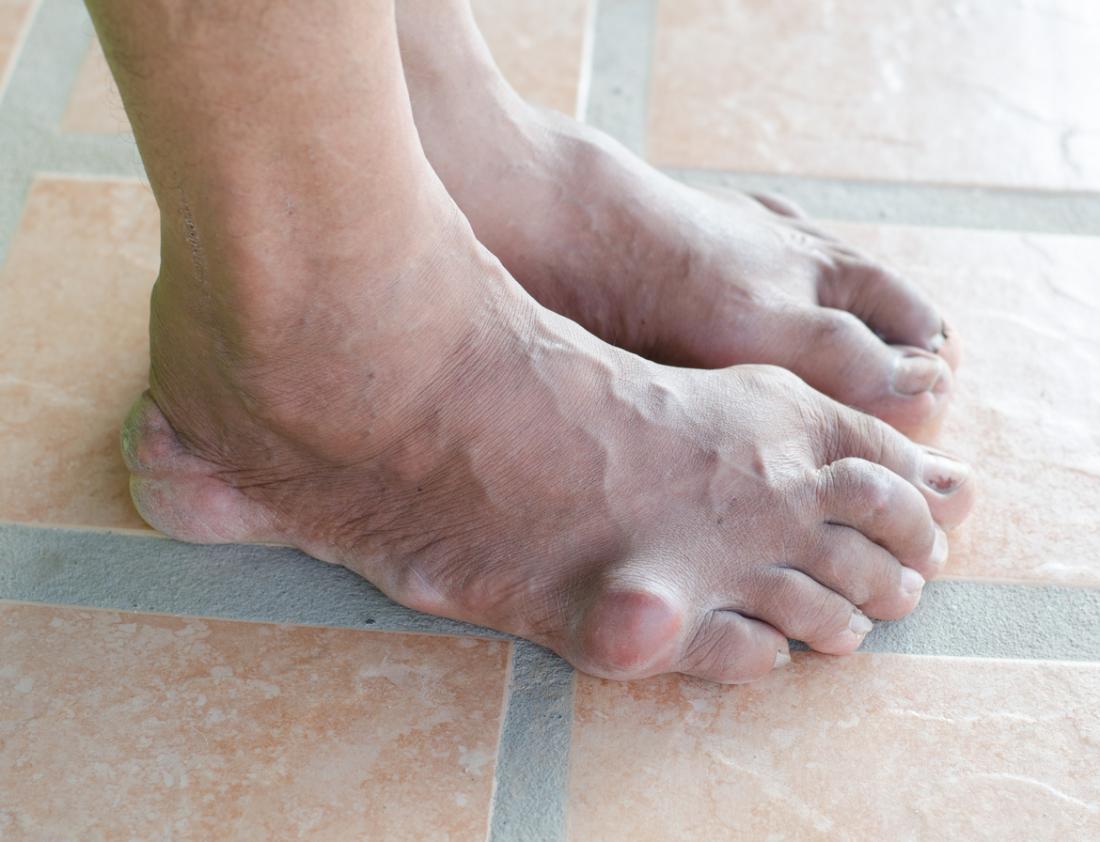
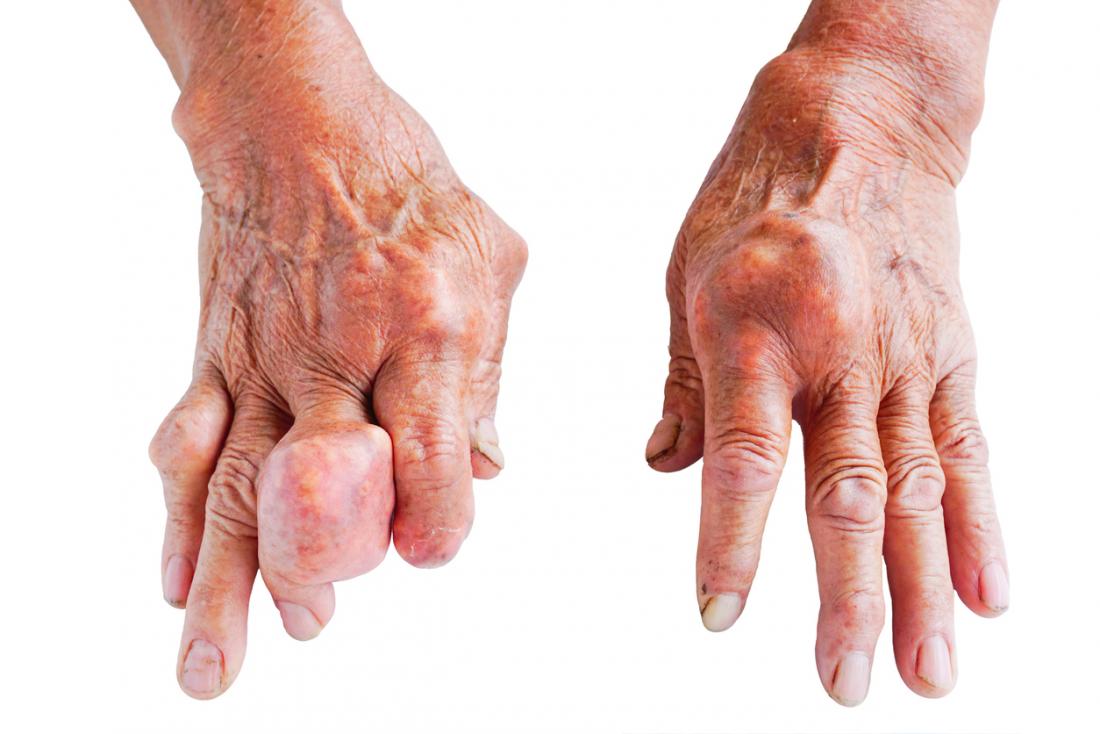
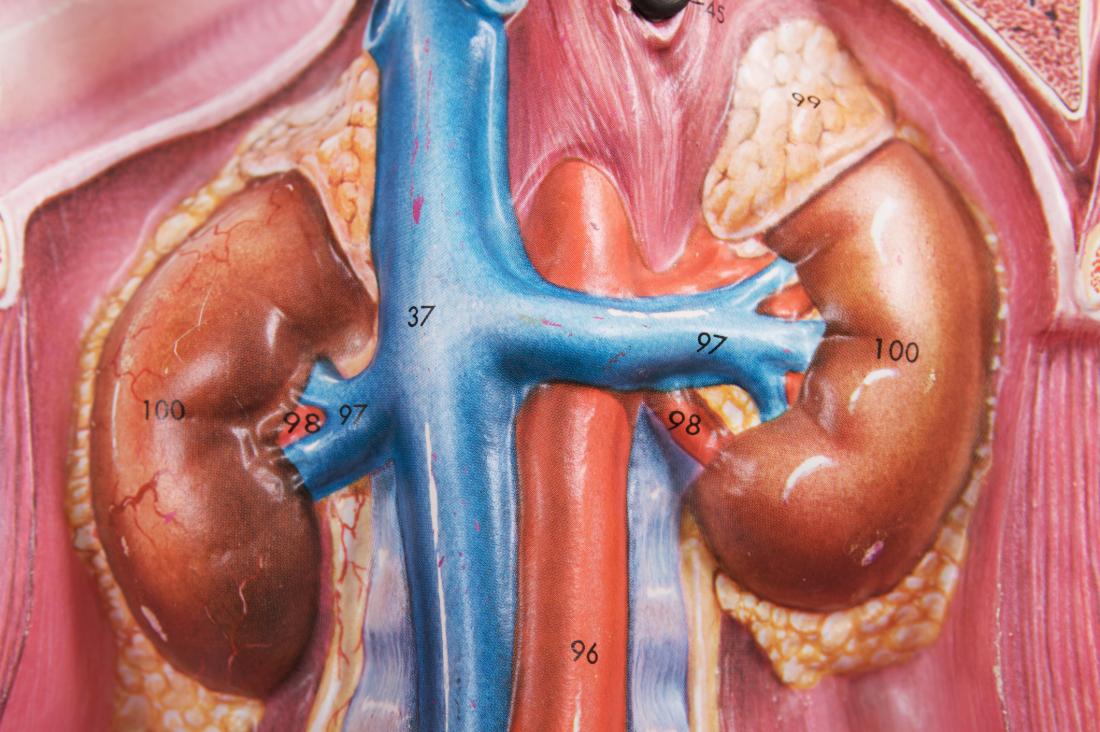
A Organização Mundial de Saúde (OMS) define cuidados paliativos como a prevenção e o alívio do sofrimento de pacientes adultos e pediátricos e de suas famílias, que enfrentam os problemas associados a doenças potencialmente fatais. Esses problemas incluem o sofrimento físico, psicológico, social e espiritual dos pacientes e de seus familiares.
Para a OMS, os cuidados paliativos:
- Proporcionam alívio da dor e de outros sintomas angustiantes;
- Afirmam a vida e consideram a morte como um processo normal;
- Não pretendem apressar ou adiar a morte;
- Integram os aspectos psicológicos e espirituais do atendimento ao paciente;
- Oferecem um sistema de apoio para ajudar os pacientes a viver o mais ativamente possível até a morte e para auxiliar a família durante a doença do paciente e em seu próprio luto;
- Usam uma abordagem de equipe para atender às necessidades dos pacientes e de suas famílias, incluindo o aconselhamento do luto, se indicado;
- Melhoram a qualidade de vida, e também podem influenciar positivamente o curso da doença;
- São aplicáveis no início do curso da doença, em conjunto com outras terapias que se destinam a prolongar a vida, como a quimioterapia ou a radioterapia, e incluem as investigações necessárias para melhor compreender e gerir complicações clínicas angustiantes.
Cuidados Paliativos em Pediatria
Os cuidados paliativos em pediatria (CPP) evoluíram do movimento de cuidados paliativos para adultos, estabelecido nas décadas de 1970 e 19803. Representam um campo especial, embora intimamente relacionado aos cuidados paliativos de adultos (CPA). Os CCP, segundo a OMS, são definidos como o cuidado ativo total do corpo, mente e espírito da criança, e isso envolve também dar apoio à família. De acordo com a OMS:
- CPP começam quando a doença é diagnosticada e continuam independentemente de a criança receber ou não tratamento direcionado à doença;
- Os profissionais de saúde devem avaliar e aliviar o sofrimento físico, psicológico e social de uma criança;
- CPP eficazes requerem uma ampla abordagem multidisciplinar que inclua a família e faça uso dos recursos disponíveis na comunidade; podem ser implementados com sucesso mesmo que os recursos sejam limitados.
- Podem ser fornecidos em instalações de cuidados terciários, em centros de saúde comunitários e até em lares de crianças.
Para os profissionais que trabalham em pediatria, é incontestável que uma criança não é simplesmente um adulto em miniatura. Isto é bastante verdadeiro em CPP, já que os cuidadores devem se esforçar para abordar os aspectos mais amplos das necessidades psicossociais e educacionais de uma criança. No entanto, os conhecimentos alcançados em cuidados paliativos para adultos são extremamente relevantes e devem ser bem aproveitados, a começar pela vantagem inicial de 40 ou 50 anos na frente.
Os princípios da medicina paliativa incluem uma abordagem holística focada no paciente, desenvolvimento e confiança em evidências robustas para tomar decisões terapêuticas racionais. E uma ênfase constante na combinação desses dois fatores para equilibrar a carga e os benefícios, assegurando que os melhores interesses do indivíduo permaneçam preservados. Estes tornam-se particularmente importantes em cuidados paliativos, quando o objetivo do tratamento se torna a manutenção da qualidade de vida.
Algumas similaridades e diferenças entre CPA e CPP estão descritas nos Quadros 1 e 2.


Indicações
Os CPP são idealmente integrados ao cuidado de qualquer criança com uma condição potencialmente fatal e são indicados e observados nas seguintes condições citadas nos Quadros 3 e 4.


Dor e outros sintomas em CPP
As crianças que necessitam de CPP apresentam uma série de manifestações clínicas. As mais comuns, independentemente do diagnóstico, são dor, dispneia e fadiga. Em cuidados paliativos, há uma forte relação entre componentes físicos e psicológicos das diversas manifestações clínicas. Distúrbios do sono, ansiedade, tristeza e depressão podem ter impacto significativo na dor. A dor e o sofrimento repercutem não apenas no paciente, mas também em seus familiares.
O Quadro 5 descreve as manifestações clínicas mais comuns de algumas situações que exigem cuidados paliativos em pediatria

Apesar do crescimento e dos avanços significativos dos CPP nas últimas duas décadas, atualmente um grande número de hospitais infantis não possui um serviço específico ou os recursos são insuficientes.
Para Friedrichsdorf e Bruera (2018), a implementação de um serviço de CPP passa em geral por quatro etapas. Isso deve ser antecipado, e um plano de ação pode incluir:
- Negação: documentar as necessidades não atendidas, realizar pesquisas entre funcionários, pacientes e provedores;
- Palliphobia: estreita colaboração com colegas; planejamento disciplinado, rápida resolução de conflitos;
- Pallilalia: documentação do valor dos CPP para a liderança; grandes rodadas por especialistas em campo e revisão externa;
- Paliativo: “faça o bem e fale sobre isso” – inovadores clínicos e administrativos devem estar envolvidos no desenvolvimento do programa;
- Financiamento seguro: “verifique se sua paixão está conectada ao sistema de pagamento de alguém”.
Os CPP de alta qualidade para crianças com doenças graves agora são um padrão esperado da medicina. No entanto, mesmo em ambientes ricos em recursos, ainda existem barreiras significativas para alcançar atendimento ideal relacionado à falta de educação formal, questões de reembolso, impacto emocional ao se cuidar de uma criança moribunda e, o mais importante, falta de equipes interdisciplinares de CPP.
O tratamento deve se concentrar, sempre que possível, nos esforços contínuos para controlar a doença subjacente. Ao mesmo tempo, as crianças e suas famílias devem ter acesso a cuidados interdisciplinares visando a promover o bem-estar físico, psicológico e espiritual ideal. Mitos e conceitos errôneos persistentes levam ao controle inadequado dos sintomas em crianças com doenças que limitam a vida.
Para Friedrichsdorf e Bruera (2018), os CPP defendem a prestação de cuidados de conforto, dor e gerenciamento de sintomas simultaneamente com os tratamentos direcionados à doença.